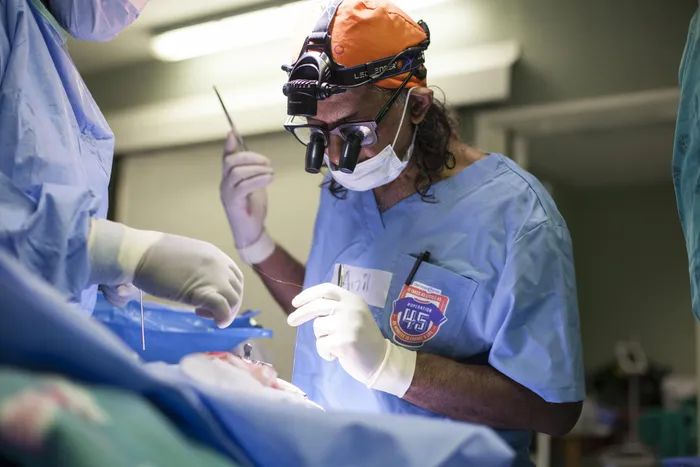
Professor Anil Madaree, the Medical Director of Operation Smile South Africa in theatre.
Image: Supplied.
TWENTY years after its first surgical programme, Operation Smile South Africa (OSSA) continues to change lives across the continent, giving hope to children and adults born with cleft lips and palates.
It all started in Empangeni in northern KZN in 2006 when almost 100 people arrived at its first surgical programme; 59 eventually received free cleft surgery that transformed their lives forever.
Professor Anil Madaree, the Medical Director of Operation Smile South Africa, says the impact of cleft surgery is immediate and profound.
“You see it on the patient’s face, on the family’s face. It’s the satisfaction that you can make a meaningful change. There’s nothing quite like it in surgery,” he said.
He says for some families the transformation goes beyond appearance. “One mother told me, for the first time, I could kiss my child,” Madaree recalls. “Before the surgery, her lips were apart. She couldn’t.”
Through OSSA, Madaree who heads the Department of Plastic and Reconstructive Surgery at the Nelson R Mandela School of Medicine at UKZN and has served as President of the Colleges of Medicine of South Africa since 2010, is at the helm of one of Africa’s most impactful volunteer-driven healthcare initiatives.
To date, the organisation has performed over 6 000 cleft lip and palate surgeries, supported by more than 150 volunteer medical professionals, including surgeons, nurses, anaesthetists, speech therapists and social workers.
He says the impact of a cleft lip is largely social and, once it’s repaired, patients are more likely to be accepted and access opportunities such as employment.
A cleft palate, however, can have more serious medical consequences. “You can't eat properly, you regurgitate and recurrent ear infections are common,” he said. “There's a social impact because if you've got a cleft palate, you can't speak, you speak very funny, no one can understand you.”
OSSA has worked across sub-Saharan Africa, changing lives in communities where specialised surgical care is often difficult to access, including the Democratic Republic of the Congo, Mozambique, Ghana, Kenya, Madagascar, Rwanda and Malawi.
Madaree stresses that the medical side of cleft care is just as critical as the social impact. Lip repairs are usually performed within the first three to four months after birth, while palates are best repaired before the first year to support normal speech development. “Even if you do the surgery later, at 50, 60, or even 70 years old, there’s still a meaningful improvement,” he said.
While OSSA is still far from its goal of treating all children born with cleft palates, progress is being made.
He has called for public support to help fund the work, saying large teams are needed for surgical missions, all driven by volunteers — from surgeons and biomedical engineers to social workers — to ensure patients receive safe, high-quality treatment.
Madaree says cleft lip and palate surgery is not just cosmetic but has a profound impact on the daily lives of patients and their families, often shifting them from being shunned to being accepted in society.
“I've done a number of adult lips, you know, like patients who are from 18 to 70 or so. And you can see once you do the repair, they look at the mirror and they can't recognize themselves because they've been used to seeing this face for years.”
He recalls a father in Madagascar who walked for days with his three children, selling his belongings just to reach a surgical programme. “Those are the moments that never leave you,” he said.
For Madaree, it is a reminder that the work is far from over, and that for thousands across Africa, a simple operation can mean the difference between exclusion and a chance at a full life.