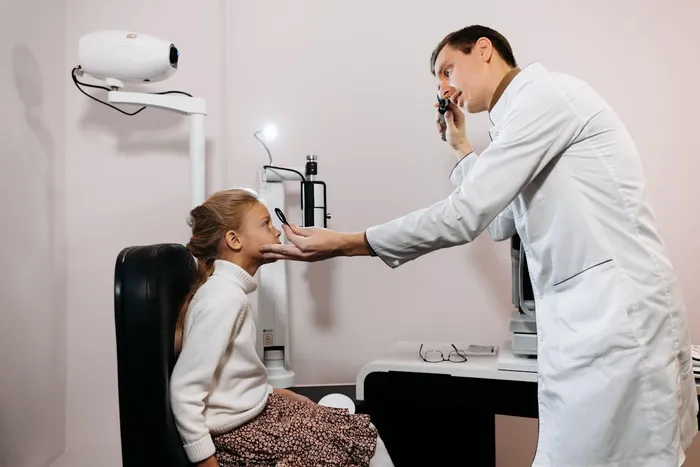
Glaucoma, a leading cause of preventable blindness in South Africa, often goes undetected until it's too late. Optometrists or ophthalmologists can perform a variety of eye tests to diagnose and determine the extent of the condition and recommend appropriate corrective measures.
Image: Pavel Danilyuk/pexels
In South Africa, glaucoma remains one of the leading causes of preventable blindness, yet a staggering 95% of those suffering from the condition are completely unaware until it is too late. Amid World Glaucoma Week (March 8-14), Dr Marissa Willemse, a specialist ophthalmologist and president of the South African Glaucoma Society (SAGS), warns that only 1 in 20 individuals know they are affected. Alarmingly, 50% will have experienced vision loss in one eye by the time they consult an ophthalmologist for the first time.
Often termed the “silent thief of sight,” glaucoma is an umbrella term for a collection of eye conditions that gradually damage the optic nerve, which is responsible for transmitting visual information from the eye to the brain. Untreated, this pressure can result in irreversible damage and eventual blindness. However, Dr Willemse emphasises that glaucoma is more than just an issue of vision; it can severely undermine daily living, affecting individuals’ independence, work, mobility and mental health long before the realisation of an issue emerges.
“Vision loss from glaucoma often starts in the periphery, creating gaps in vision that go unnoticed until they interfere with everyday activities,” Dr Willemse explains. “Even early vision loss can have significant impacts on daily routines: driving, reading, using digital devices, cooking, or navigating unfamiliar spaces.” These disruptions can lead to feelings of anxiety, depression and even social isolation, profoundly affecting an individual's quality of life.
Statistics reveal a troubling trend; in Sub-Saharan Africa, around 4.16% of the population aged 40 and above struggle with glaucoma, with the incidence reported as being higher among black individuals (5–7%) compared to their Caucasian counterparts (3–5%). The fight against this condition is further complicated by a lack of awareness, delayed diagnoses, poor follow-ups, and low compliance with treatment regimens.
Dr Willemse underscores the critical need for greater awareness surrounding glaucoma, as it often exhibits no noticeable symptoms in its early stages. As intraocular pressure escalates, damage to the optic nerve occurs, leading to progressive vision loss. By the time patients notice warning signs — such as gradual loss of peripheral vision or blurred sight — it is frequently already too late to reverse damage.
The risk factors for developing glaucoma are varied, and regular check-ups with an ophthalmologist are imperative for early detection. Key factors include:
Symptoms
Symptoms tend to manifest gradually, and include:
Screening recommendations suggest individuals under 40 undergo screenings every 2-4 years, those aged 40 to 60 every 2-3 years, and individuals over 60 annually. Screening methods typically involve comprehensive eye examinations, including:
Upon completing screening, an ophthalmologist will establish a tailored treatment plan aimed at lowering intraocular pressure to prevent further optic nerve damage. Common treatments include:
Dr Willemse calls for increased awareness of glaucoma, advocating for regular eye examinations and early detection. Access to comprehensive eye care services, particularly in under-resourced communities, is vital for managing this condition and preserving patients’ vision.
IOS
Related Topics: